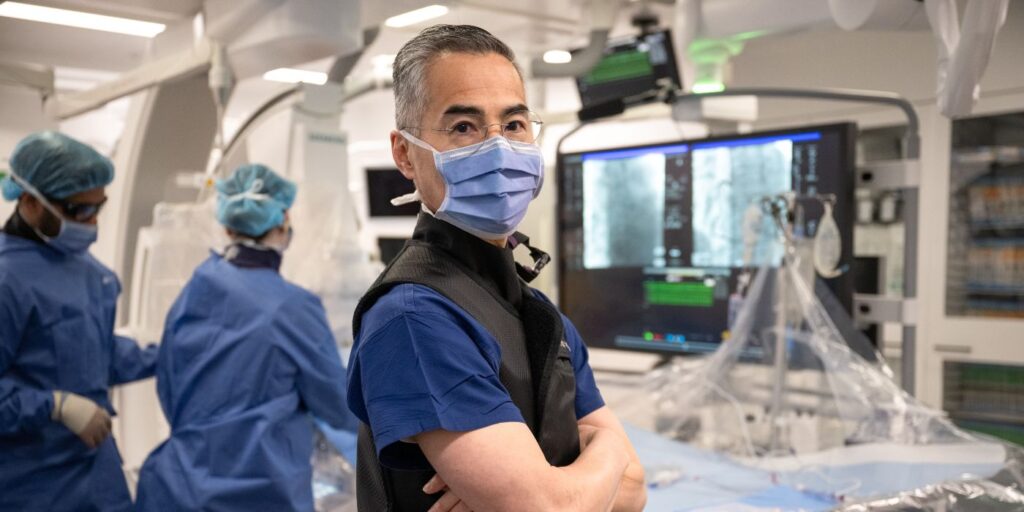
‘People who identify as part of the LGBTIQA+ community have historically been marginalised and scrutinised by the wider society. They can be more protective and hesitate to disclose their gender identity or sexual orientation in day-to-day life,’ says Dr David Colón Cabrera, Acting Clinic Manager, the current Program and Research Officer and Administration Team Leader at the Gender Clinic, and Deputy Chair of the LGBTIQA+ subcommittee.
Our Gender Clinic has been at the forefront of specialised services that understand the specific challenges that transgender, gender diverse and non-binary patients face in our healthcare system.


‘Information about a patient’s preferred name, name used for their Medicare record, and their pronouns, gender identity and sex assigned at birth can be wrongly assumed in or missing in case notes or patient referrals through the healthcare system. Herein lies the risk that patients could be misidentified or end up receiving inappropriate treatment.’
Based at the Victorian Pride Centre, the Gender Clinic has been providing a unique statewide service that provides individualised, person-centred care for transgender, gender diverse and non-binary people, their families, partners and the community. Celebrating its 50th birthday last year, it’s the oldest and largest gender-affirming health service in Australia.
The education and training delivered by the Gender Clinic is important not only within Monash Health but with other community partners, healthcare providers and advocacy groups, to reduce the risk of patient misidentification across the healthcare system.
‘The Gender Clinic team delivers tailored sessions about gender-affirming care for a number of teams, including Mental Health units and clinician orientations. We’ve also presented at Medical Grand Rounds,’ shares Jessica Shillinglaw, Acting Clinic Manager of the Gender Clinic and Discipline Senior Speech Pathologist with the Adult Mental Health Program.
Graduate Mental Health Nurses Kamaljeet Kaur and Garry Dulang recently benefited from one of the Gender Clinic’s training sessions.
‘As a first-year graduate nurse working on the floor, I care for many consumers from different backgrounds, including people who are gender diverse,’ says Kamaljeet, who is a first-year graduate nurse working on the floor.
‘Since attending the training, I have become more mindful about using inclusive language and asking rather than assuming. I think this has helped me provide more respectful and person-centred care and create a safer environment for consumers to feel comfortable and supported.’
Garry felt similarly, emphasising the importance of effective communication.
‘Assumptions take away the autonomy and the voice of the patient and can lead to situations ranging from inconvenient to life-altering. Instead of assuming, asking questions respectfully can give a patient the opportunity to share important information about their health and care. This is especially important for gender-diverse patients, whose appearance may not reflect their experience,’ says Garry.
‘Avoiding assumptions is not limited to this demographic. By taking the time to communicate effectively, even if it might feel awkward for a few moments, we make our care inclusive of all. This principle guides me to continually improve my nursing practice as a graduate nurse.’

At Monash Health, our vision is to ensure we lead the way in respecting, celebrating and warmly welcoming people of every gender, gender identity, intersex variation and sexual orientation. We listen to our community to better understand their needs and ensure everyone feels safe and included and aim to foster a unifying culture that practices LGBTIQA+ awareness and support.
If you or your team are interested in gender-affirming healthcare training or support, contact our Gender Clinic to discuss your needs and requirements. Visit the Gender Clinic page on the Monash Health website.